Gastroenterology
Gastroenterology is the medical specialty dedicated to the study of the functioning and diseases of the entire digestive system, including the oesophagus, stomach, small intestine, colon and rectum, anus, pancreas, gallbladder, bile ducts and liver.
The Gastroenterology Units of the HPA Saúde Group are supported by highly specialised clinical teams with experience in all areas of the digestive system, ensuring a comprehensive and rigorous approach to the assessment of gastrointestinal diseases. Their practice is guided by high standards of clinical safety, accessibility to healthcare and respect for patient privacy, guaranteeing an environment of trust throughout all stages of care.
- Dra. Ana Margarida Vieira
- Dr. André Sancho Ramos
- Dr. Bruno Peixe
- Dra. Helena Tavares de Sousa
- Dra. Maria Margarida Sampaio
- Dra. Patrícia Queirós
- Dra. Ana Rita Herculano
- Dr. André Sancho Ramos
- Dr. Diamantino Sousa
- Dr. Francisco Açucena
- Dr. Horácio Guerreiro
- Dr. Mário César
- Dr. Horácio Guerreiro
- Dra. Carla Sousa Andrade
- Dra. Isabel Jardim
- Dr. Luís Jasmins
- Dr. Nuno Ladeira
- Dra. Rosa Neto da Silva
- Dr. Vítor Magno Pereira
- Dra. Carla Sousa Andrade
- Dra. Isabel Jardim
- Dr. Luís Jasmins
- Dr. Nuno Ladeira
- Dra. Rosa Neto da Silva
Hospital Particular do Algarve - Alvor
Hospital Particular do Algarve - Gambelas
Hospital São Camilo - Portimão
Clínica Particular SIIPEMOR - S. Brás Alportel
Hospital Particular da Madeira
Madeira Medical Center
From diagnosis to treatment, patients are continuously and comprehensively supported by a multidisciplinary team that works in a coordinated manner at all stages of the clinical process. The units perform both routine and urgent procedures, ensuring an effective, timely and appropriate response to different clinical needs.
Gastroenterology is a specialty oriented towards innovation, integrating advanced techniques and increasingly safe, effective and minimally invasive approaches. Our clinical practice prioritises preventive care, focusing on anticipating needs and responding appropriately to each patient’s concerns, thereby promoting healthcare excellence and person-centred care.
The HPA Saúde Group also offers high-resolution imaging technology and artificial intelligence systems, enabling the early detection of lesions in the digestive tract and increasing diagnostic accuracy and effectiveness. It also provides advanced endoscopic techniques, such as endoscopic submucosal dissection and peroral endoscopic myotomy (POEM), which allow the treatment of tumours and other digestive tract conditions while avoiding more invasive approaches, namely conventional surgery, and promoting safer and faster recovery for patients.
Main conditions

Achalasia
Achalasia is a rare disease of the oesophagus, characterised by difficulty in the passage of food from the oesophagus to the stomach. It results from abnormal oesophageal motility and inadequate relaxation of the lower oesophageal sphincter, which remains excessively contracted.
Ulcerative Colitis
Ulcerative colitis, also known as ulcerative proctocolitis, is a chronic inflammatory disease of the large intestine, characterised by continuous inflammation of the mucosa of the colon and rectum, which may lead to ulcer formation. It mainly presents with gastrointestinal symptoms such as diarrhoea, rectal bleeding and abdominal pain, and belongs to the group of inflammatory bowel diseases, alongside Crohn’s disease.

Anal and Perianal Condylomas
Anal and perianal condylomas are wart-like lesions, most commonly caused by infection with the Human Papillomavirus (HPV). These lesions may develop inside the anus or around the perianal area, causing physical and aesthetic discomfort. Transmission occurs primarily through sexual contact.
Colonic Diverticulosis
Diverticulosis is a condition characterised by the presence of small pouches in the lining of the large intestine, known as diverticula. It is more common in industrialised countries, where typical diets are low in dietary fibre. Fibre, found in fruit, vegetables, seeds and cereals, is not digested by the gastrointestinal tract but plays an essential role in forming softer stools, facilitating bowel movements and preventing constipation.

Coeliac Disease
Coeliac disease is an autoimmune condition triggered by the consumption of gluten; a protein found in foods such as bread, biscuits, pasta and certain cereals. When genetically predisposed individuals ingest gluten, the immune system reacts, causing inflammation and atrophy of the villi in the small intestine. This damages the intestine’s ability to absorb nutrients, vitamins, minerals and water. Malabsorption may lead to reduced bone density, infertility, fatigue, neurological disorders and even certain types of cancer.

Crohn’s Disease
Crohn’s disease is a chronic inflammatory bowel disease, likely of autoimmune origin, characterised by inflammation of the digestive tract, which may cause ulcers and bleeding. It most commonly affects the colon and terminal ileum, but can involve any part of the gastrointestinal tract, from the mouth to the anus.
Inflammatory Bowel Disease
Inflammatory Bowel Disease (IBD) is a chronic condition of the digestive system characterised by persistent intestinal inflammation, which may cause redness, swelling and ulcer formation. It mainly includes two conditions: ulcerative colitis and Crohn’s disease. When a clear distinction between the two cannot be made, it is referred to as indeterminate colitis.
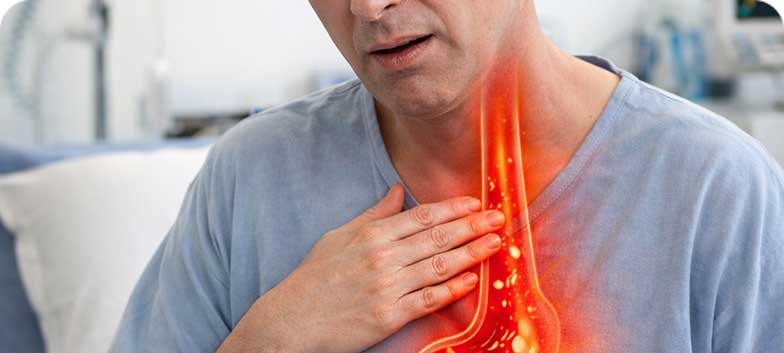
Oesophagitis
Oesophagitis is inflammation of the oesophagus, the tube that connects the throat to the stomach. It may cause pain, difficulty swallowing, reflux symptoms or chest pain. Inflammation occurs when the immune system reacts to infections, allergies, injury or erosive substances such as gastric acid or certain medications. Chronic acid reflux is one of the most common causes, although other less common types exist.

Anal Fibromas
Anal fibromas are benign fibrous tissue growths that usually develop in the anal region. They are often associated with inflammatory processes or chronic proctological conditions. In most cases, anal fibromas are asymptomatic and do not cause problems.
However, they may cause pain, discomfort, local inflammation or difficulty with personal hygiene. In such cases, removal may be indicated. The procedure is usually minimally invasive and performed during a Proctology consultation, allowing symptom relief and prevention of complications.
Fatty Liver Disease (Hepatic Steatosis)
Fatty liver disease, or hepatic steatosis, is a condition characterised by the accumulation of fat within liver cells. The liver plays a vital role in digestion, nutrient metabolism, detoxification and regulation of blood clotting. When fat content exceeds 5% to 10% of the liver’s weight, the condition may develop. In Portugal, approximately 15% of adults are affected, while globally prevalence reaches 20% to 30%, with a higher incidence in adult men and postmenopausal women.
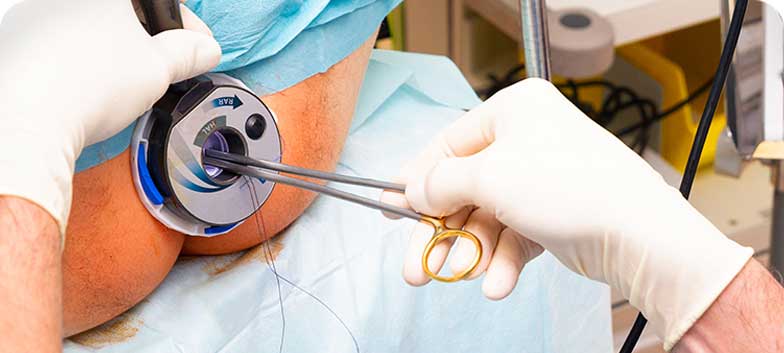
Anal Fistula
An anal fistula is an abnormal tract that forms between the anal canal and the skin surface, usually in the perianal region. It may be simple, with a single tract, or complex, with multiple secondary tracts. Anal fistulas do not heal spontaneously and usually require medical or surgical intervention. They are more common in adult men around the age of 40, while in children they are more often congenital.

Anal Fissure
An anal fissure is a small tear in the mucosa lining the anus. It is usually located in the posterior midline, but in women it may occur in the anterior midline due to anatomical differences. It can occur at any age and affects men and women equally. Fissures may be acute, when they appear suddenly, or chronic, when they persist or recur over time.
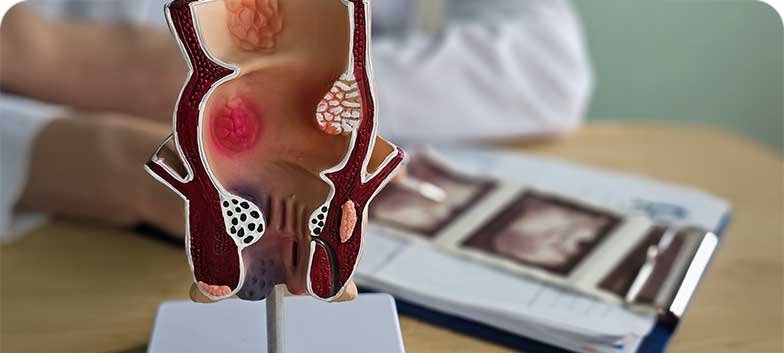
Haemorrhoids
Haemorrhoids are dilated veins located in the lower rectum and anus. They may be internal, developing inside the anus, or external, located in the skin around the anus. In some cases, both types coexist.

Hepatitis
Hepatitis is the inflammation of liver cells, an organ essential for digestion, metabolism and detoxification of the body. It can have several causes, including viruses (A, B, C, D and E), immune system disorders (autoimmune hepatitis), alcohol or drug consumption (toxic hepatitis), and fat accumulation in the liver (steatohepatitis).
Helicobacter pylori Infection
Helicobacter pylori (H. pylori) infection occurs when this bacterium colonises the stomach, usually during childhood. It is very common, affecting approximately two-thirds of the world’s population. In most cases, the presence of the bacterium causes no symptoms, but it may lead to the development of peptic ulcers, which are sores or bleeding in the lining of the stomach (gastric ulcer) or the first part of the small intestine (duodenal ulcer).
Gallbladder Stones (Cholelithiasis)
Gallbladder stones, or cholelithiasis, refer to the presence of calculi (“stones”) in the gallbladder, a small organ located beneath the liver that stores bile. After meals, the gallbladder contracts and releases bile into the small intestine, aiding fat digestion.

Constipation
Intestinal constipation, commonly referred to as constipation or a “lazy bowel”, is a frequent condition that can affect people of all ages. Its definition may vary from person to person, but it is generally characterised by infrequent bowel movements (fewer than three per week), difficulty passing stools, hard stools, or a sensation of incomplete bowel emptying.
Pancreatite
Pancreatitis is inflammation of the pancreas, an organ that produces digestive enzymes (exocrine pancreas) and hormones such as insulin (endocrine pancreas), which are essential for glucose metabolism. It may occur in an acute or chronic form, with different symptoms and clinical courses.

Intestinal Polyps
Intestinal polyps are lesions that protrude from the inner wall of the intestine into its lumen. They are more common in the colon and rectum but may occur in any segment of the digestive tract, such as the small intestine, stomach or oesophagus. These lesions vary in number, size, shape and histological type. Most polyps are isolated, but some individuals develop multiple polyps, particularly in hereditary conditions known as intestinal polyposis syndromes.
Gastro-oesophageal Reflux Disease (GERD)
Gastro-oesophageal reflux disease is a digestive disorder that occurs when acidic stomach contents reflux into the oesophagus, causing symptoms such as heartburn, a sensation of fullness and frequent belching. Frequently associated with obesity and smoking, it affects approximately 15–20% of the population. The main cause is dysfunction of the lower oesophageal sphincter, the valve that prevents gastric contents from flowing back into the oesophagus, and it may be exacerbated by factors such as increased intra-abdominal pressure, poor dietary habits, smoking and pregnancy.

Irritable Bowel Syndrome
Irritable bowel syndrome (IBS) is a functional disorder of the digestive tract characterised by a set of recurrent symptoms that significantly affect quality of life. IBS may also be referred to as colitis, nervous bowel, spastic colon or spastic bowel.

Gastric Ulcer
A gastric ulcer, also known as a stomach ulcer, is a lesion that forms in the mucosal lining of the stomach and, in some cases, may progress to rupture or bleeding. These lesions arise when the protective mucus layer of the stomach is reduced, allowing digestive acids to damage the underlying tissues. Ulcers may be asymptomatic in their early stages; however, if left untreated, they can cause intense abdominal pain, discomfort and serious complications. The term peptic ulcer disease includes both gastric ulcers and ulcers that occur in the first part of the small intestine, the duodenum.
Main Diagnostic Examinations
Anoscopy
Anoscopy is an examination that allows direct evaluation of the anus, anal canal and rectal ampulla. It is performed using an anoscope, enabling the physician to identify inflammation, haemorrhoids, fissures, fistulas, abscesses, prolapse or suspicious lesions, and, if necessary, to collect small tissue samples (biopsies).
The examination is generally well tolerated, causing only mild pressure or an urge to defecate, and rarely results in complications, although mild bleeding may occur in isolated cases. In most situations, no prior preparation is required, although a cleansing enema may occasionally be recommended.
Endoscopic Retrograde Cholangiopancreatography (ERCP)
ERCP is an advanced endoscopic procedure used to treat disorders of the bile ducts and pancreas, such as obstructions caused by gallstones, tumours or inflammation. Symptoms indicating the need for ERCP include abdominal pain, jaundice, fever, itching or episodes of pancreatitis.
The procedure is performed under deep sedation or general anaesthesia, with an endoscope introduced through the mouth to the duodenum, allowing contrast injection, visualisation of the ducts and therapeutic interventions such as stone removal, stent placement, sphincterotomy and biopsies.
Essentially, ERCP allows treatment of biliary and pancreatic conditions while avoiding surgery in many cases.
Before the examination, the patient must undergo blood tests, an ECG if necessary, and inform the physician about medications such as anticoagulants or the presence of a pacemaker.
After the procedure, the patient is monitored until full recovery from sedation and, in most cases, remains hospitalised for at least 24 hours. ERCP is always preceded by a medical consultation with a gastroenterologist, who evaluates, explains and follows the entire process.
Colonoscopy
Colonoscopy, also known as lower gastrointestinal endoscopy, is an examination that allows visualisation of the entire large intestine (colon and rectum) and, in some cases, part of the small intestine. It is performed by a gastroenterologist using a thin, flexible tube called a colonoscope, which transmits images to a monitor. The examination identifies inflammation, tumours, polyps, bleeding and other intestinal abnormalities and is widely used for colorectal cancer screening.
Biopsies or minor therapeutic interventions, such as polyp removal or bleeding control, may be performed during the examination. Colonoscopy may be carried out with or without sedation, depending on the clinical situation and patient tolerance. Bowel preparation is essential and involves a specific diet and the intake of laxative solutions to cleanse the intestine.
After colonoscopy, mild abdominal discomfort or bloating due to air insufflation is common. Complications are rare but may include intestinal perforation, bleeding or reactions to anaesthesia. Patients should inform their doctor if they experience severe pain, fever, bleeding or breathing difficulties.
Endoscopic Ultrasound (EUS)
Endoscopic ultrasound combines endoscopy and ultrasonography, allowing detailed visualisation of the gastrointestinal wall and adjacent structures such as the pancreas and bile ducts. It is performed by a gastroenterologist using a thin, flexible echoendoscope introduced through the mouth or anus, depending on the area under investigation.
EUS enables assessment of lesions, tumours and other abnormalities of the digestive system and allows highly accurate biopsies. The examination duration varies, typically between 15 and 60 minutes. Upper EUS is usually performed under sedation, whereas lower EUS may be carried out without anaesthesia.
After the examination, mild abdominal discomfort or gas may occur, but recovery is rapid and patients can usually return home the same day.
Transient Hepatic Elastography (FibroScan)
Transient hepatic elastography, also known as FibroScan, is a fast, painless and non-invasive examination that assesses liver stiffness and fat content (steatosis). It is used to detect liver fibrosis caused by alcohol-related disease, hepatitis, obesity, metabolic syndrome or autoimmune disorders, helping to predict the risk of cirrhosis and severe liver complications.
The examination uses sound waves that pass through the liver to measure tissue elasticity. The patient lies on their back with the right arm raised, and a gel is applied to the skin to facilitate probe contact. The procedure takes approximately 10 minutes and allows immediate resumption of normal activities.
Results indicate whether the liver is normal, fatty, fibrotic or cirrhotic and are expressed in kilopascals (kPa) for stiffness and CAP for fat content. FibroScan is indicated for individuals with suspected liver disease, treatment monitoring or risk assessment, but has limitations in obese patients, those with ascites, pregnant women or individuals with certain cardiac devices.
Upper Gastrointestinal Endoscopy
Upper gastrointestinal endoscopy (OGD) allows visualisation of the oesophagus, stomach and duodenum using a thin, flexible endoscope that transmits images to a monitor. It is performed by a gastroenterologist to investigate symptoms such as abdominal pain, heartburn, vomiting or difficulty swallowing, and to diagnose bleeding, ulcers, inflammation or tumours.
The examination may include biopsies or minor therapeutic interventions, such as polyp removal or bleeding control. It can be performed with local anaesthesia or sedation to ensure patient comfort. Prior to the examination, the stomach must be empty, and patients should inform the doctor about medications, allergies or medical conditions.
After OGD, mild throat discomfort or a feeling of fullness may occur. Complications are rare but can include bleeding or reactions to anaesthesia. Patients should seek medical advice if severe pain, fever or difficulty swallowing develops.
Video Capsule Endoscopy
Video capsule endoscopy is a safe, non-invasive and painless diagnostic examination that allows visualisation of the entire small intestine. It is performed by swallowing a capsule containing a camera and light source, which records images as it moves through the digestive tract by natural intestinal movements. Images are captured by sensors attached to the body and later analysed by the physician. The capsule is naturally excreted in the stool within 24 to 72 hours.
It is indicated for the investigation of chronic anaemia, persistent abdominal pain, gastrointestinal bleeding of unknown origin, suspected Crohn’s disease, ulcers, neoplasms or intestinal polyposis, and to clarify findings from other examinations. The test lasts approximately 8 hours and does not allow biopsies or therapeutic procedures during this time.
Although very safe, the main risk is capsule retention in the intestine, which in rare cases may require imaging or surgical intervention. Patients should inform their doctor of allergies, pre-existing conditions and current medications prior to the examination.
Manometry
Manometry is a minimally invasive, painless examination that assesses oesophageal function by measuring the activity of the muscles responsible for transporting food from the mouth to the stomach. It is performed by introducing a thin catheter with pressure sensors through the nostrils, allowing detection of oesophageal movements and pressure patterns. The test takes approximately 20 to 30 minutes.
It is indicated for the investigation of swallowing difficulties, non-cardiac chest pain, persistent heartburn or reflux resistant to treatment, and for preoperative evaluation prior to oesophageal or gastric surgery. It also aids in diagnosing oesophageal spasms and other motility disorders.
Before the examination, the stomach must be empty, avoiding food and liquids for at least 6 hours. The test is generally well tolerated, causing only mild throat discomfort that resolves within a few hours. Normal activities and diet can usually be resumed immediately after manometry, unless otherwise advised.
Flexible Sigmoidoscopy
Flexible sigmoidoscopy allows visualisation of the distal 30 to 40 cm of the large intestine, including the rectum and sigmoid colon. It is performed by a gastroenterologist using a thin, flexible sigmoidoscope that transmits images to a monitor. Small tissue samples (biopsies) may be taken during the procedure.
The examination is indicated for the investigation of rectal bleeding, abdominal pain, changes in bowel habits, chronic diarrhoea or suspected intestinal diseases such as polyps, ulcerative colitis, Crohn’s disease or haemorrhoids. Preparation involves bowel emptying with enemas or laxatives. The procedure is usually quick (around 10 minutes) and well tolerated, with less discomfort and fewer risks than colonoscopy.
After the examination, gas, cramping or mild abdominal discomfort may occur, but patients can resume their normal diet and activities immediately.
Clinical Team
HPA Gastroenterologists











